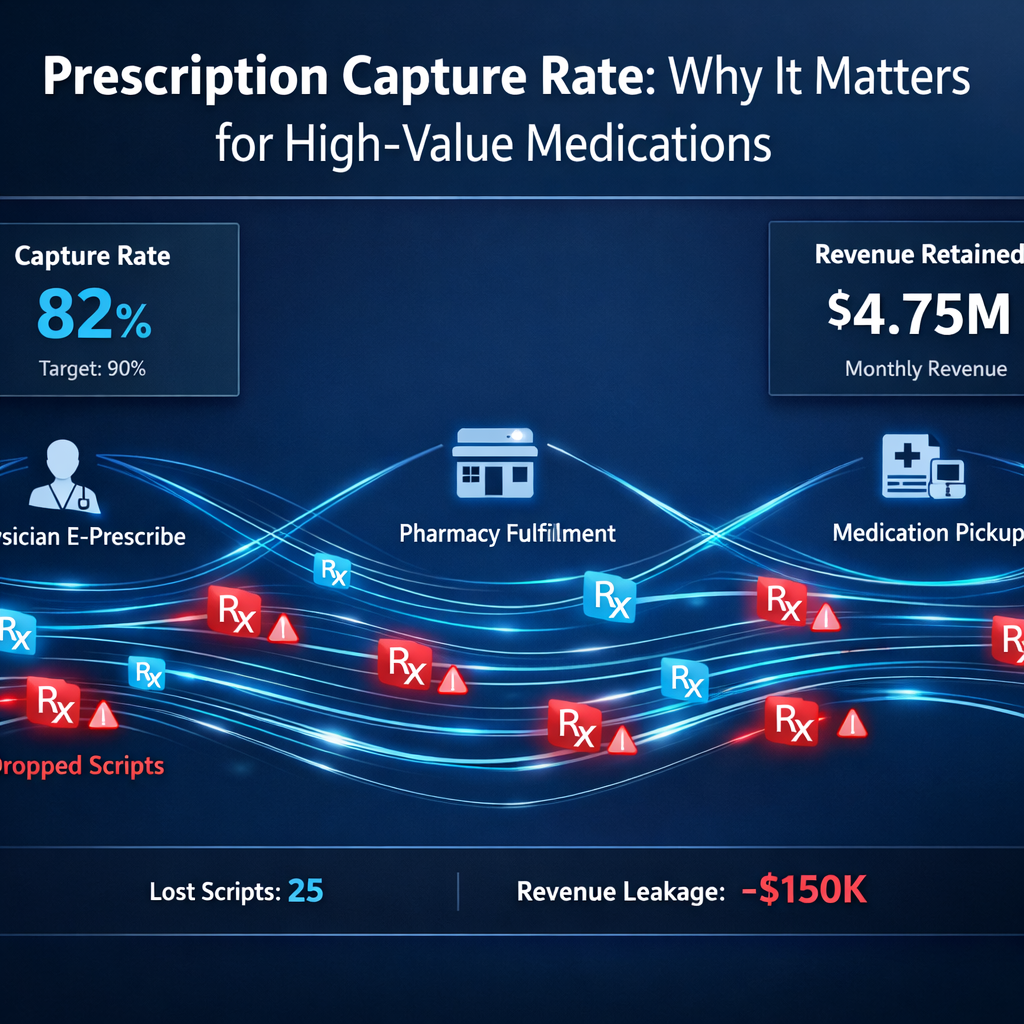
For health systems, prescription capture rate is more than a performance metric. It is a direct indicator of financial stability, operational coordination, and continuity of therapy for high-value medications.
As specialty and complex therapies account for a growing share of overall drug spend, even minor breakdowns in capture can result in substantial revenue leakage. Yet many hospital pharmacies still lack the visibility needed to monitor medication across the full lifecycle.
Improving prescription capture rate requires proactive analytics, cross-functional alignment, and real-time insight. These capabilities sit at the core of Quva BrightStream’s Script Revenue Capture solution, which helps organizations protect high-value script revenue before it is lost.
Understanding Prescription Capture Rate in Hospital Pharmacies
What prescription capture rate means for health systems
Prescription capture rate refers to the percentage of eligible prescriptions that are successfully filled within a health system’s pharmacy network instead of being transferred externally or remaining unfilled.
For integrated delivery networks, this metric directly influences revenue performance, margin stability, and forecasting accuracy. A low capture rate often signals fragmentation in operational processes that may otherwise go unnoticed.
Why high-value and specialty medications are most at risk
High-cost and specialty medications frequently require additional coordination, documentation, and communication between departments. Each additional workflow step increases the potential for delay or leakage.
Because these therapies represent significant financial value per medication, even a small drop in capture rate can have an outsized impact on pharmacy revenue and service line performance. Without structured monitoring, these high-value opportunities are particularly vulnerable.
How missed capture affects revenue, inventory, and access
Missed capture has downstream effects that extend well beyond a single transaction. When medications leave the system or stall in workflow queues, the financial and operational impact compounds over time.
The consequences often include:
- Lost pharmacy revenue from high-cost therapies
- Inaccurate inventory forecasting and purchasing decisions
- Strained margins within specialty service lines
- Delays that disrupt therapy initiation and follow-up coordination
These effects can ripple across departments, creating instability in both operational planning and financial performance. Over time, repeated leakage erodes confidence in forecasting models and limits the ability to invest in growth initiatives.
Why Prescription Revenue Is Commonly Lost Across the Medication Lifecycle
Prescription leakage rarely stems from one isolated failure. Instead, it reflects fragmented systems, inconsistent workflows, payer complexity, and a lack of visibility across the care continuum.
When multiple systems and teams are involved, visibility gaps can form between handoffs. Without integrated monitoring, small delays or missed tasks accumulate into measurable revenue loss.
Revenue leakage in high-value outpatient therapies
Many of the most financially significant medications are administered in outpatient settings and covered under the medical benefit rather than the pharmacy benefit. These therapies are often high-cost, require prior authorization or step therapy, demand ongoing monitoring, and involve coordination across multiple teams.
Because the revenue cycle for these medications is longer and less transparent, leakage often occurs in less visible ways. Gaps in follow-on therapy, protocol drift, external referrals, inconsistent prescribing patterns, or patient non-adherence can all result in care — and associated reimbursement — moving outside the system. Without clear insight into where these breakdowns occur and why, health systems struggle to quantify lost revenue, prioritize recovery opportunities, or standardize processes to improve both financial performance and clinician experience.
The impact of manual processes and disconnected systems
Many health systems continue to rely on manual tracking and siloed reporting. These processes create lag between action and insight, making proactive intervention difficult.
Manual workflows often result in:
- Delayed identification of stalled medications
- Inconsistent tracking across sites and service lines
- Increased administrative burden on pharmacy teams
- Limited ability to prioritize high-value opportunities
As workload increases, the risk of oversight grows. Manual reconciliation may identify revenue loss after the fact, but it rarely prevents leakage in real time.
Fragmented data obscures where and why revenue is leaving the system
When clinical, operational, and financial data live in separate platforms, health systems lack a unified view of prescription-related revenue performance. This fragmentation makes it difficult to see not just what happened to a therapy, but whether the organization retained the associated reimbursement.
Without integrated visibility, leadership cannot clearly identify:
- Which sites of care are losing high-value therapies Whether referrals are directing patients outside the network Where protocol drift or prescribing variation is impacting retention How payer dynamics and reimbursement patterns influence revenue capture
Revenue leakage is rarely caused by a single event. It emerges from disconnected signals across the care continuum. Without a consolidated view, health systems struggle to diagnose root causes, prioritize recovery efforts, or align clinical behavior with financial strategy.
The Limitations of Traditional Approaches to Revenue Capture
Traditional revenue capture strategies are typically retrospective. They focus on identifying revenue after it has already been lost rather than preventing leakage upstream.
While audits and reconciliation processes are important for financial reporting, they are not designed to improve prescription capture rate in real time.
Reliance on retrospective reporting and manual reconciliation
Many organizations depend on end-of-month financial reports and manual cross-checks to assess performance. These methods provide visibility, but only after opportunities have passed.
Common limitations include:
- Revenue leakage being identified weeks after occurrence
- Labor-intensive reconciliation across disparate systems
- Limited insight into the root causes of capture failure
- Inability to intervene before drugs leave the network
By the time reports are finalized, recovery options may be limited or nonexistent. This reactive cycle prevents sustainable improvement.
Challenges tracking across sites and care settings
Large health systems often operate multiple hospitals, ambulatory clinics, specialty pharmacies, and infusion centers. Tracking drugs consistently across these environments is inherently complex.
Without centralized analytics, leadership may see only partial performance data at each site. This fragmentation makes enterprise-level optimization nearly impossible and obscures system-wide leakage trends.
Why pharmacies struggle to prioritize high-value opportunities
Not all medications carry equal financial impact, yet many workflows treat them similarly. When staff resources are limited, high-value scripts that require proactive follow-up may not receive additional attention.
Without structured prioritization tools, pharmacy teams are forced to manage by queue rather than by value. This limits the ability to protect specialty medication revenue effectively.
How Analytics Improve Prescription Capture Rate
Data-driven analytics shift prescription revenue capture from reactive reporting to proactive protection. Instead of discovering leakage after it occurs, organizations can identify risk earlier and intervene strategically. This shift requires centralized data, intelligent alerts, and workflow-integrated insights.
Identifying medications at risk of leakage in real time
Real-time monitoring allows pharmacy leaders to detect stalled workflows and high-value drugs that may be at risk of leaving the system.
Advanced analytics can:
- Monitor prescription status across systems and locations
- Flag delays or inactivity that indicate risk
- Surface high-cost therapies requiring follow-up
- Quantify potential revenue impact of at-risk scripts
By surfacing prioritized alerts rather than raw data, analytics platforms enable teams to act before revenue is lost. Quva’s BrightStream Script Revenue Capture solution is designed to deliver this type of actionable intelligence.
Prioritizing high-value medications for proactive follow-up
Analytics platforms can rank medications by financial impact and complexity, ensuring that limited staff time is applied strategically. This enables pharmacy teams to focus on specialty and high-margin therapies that drive overall performance.
By identifying which medications warrant immediate attention, organizations improve capture rate without increasing administrative burden.
Enabling pharmacy teams to intervene earlier and more efficiently
Centralized dashboards and structured insights streamline decision-making. Rather than searching across systems, teams can view prescription status and risk indicators in a single interface.
Earlier intervention increases the likelihood of successful capture while reducing downstream reconciliation work. Over time, this proactive model strengthens both financial and operational resilience.
Key Insights That Support Improved Prescription Capture
Data alone does not improve performance. The value lies in converting data into clear signals that guide action.
When prescription performance is tracked longitudinally, patterns begin to emerge that highlight structural weaknesses and optimization opportunities.
Visibility into prescription status across systems and locations
Enterprise-wide visibility provides clarity into where medications originate, how they move through workflows, and where leakage occurs. This consolidated view eliminates blind spots across departments and care settings.
With centralized insight, leadership can measure capture rate consistently and identify performance variation across sites.
Trends that reveal systemic leakage or workflow gaps
Over time, aggregated data reveals patterns that would otherwise remain hidden. Identifying recurring leakage points allows organizations to implement structural improvements instead of isolated fixes.
Common trends that surface include:
- Persistent capture loss within specific specialties
- Delays tied to authorization or documentation workflows
- Transfer patterns concentrated at certain facilities
- Service lines with disproportionate leakage risk
Recognizing these trends enables targeted intervention and process redesign that improves capture rate sustainably.
Actionable signals that help teams focus resources effectively
Effective analytics platforms translate complex data into ranked opportunity lists and prioritized alerts. Instead of overwhelming teams with dashboards, they surface the drugs most likely to affect revenue.
This targeted focus ensures that pharmacy teams spend time where it delivers the greatest return.
Building a Sustainable Strategy to Improve Prescription Capture Rate
Improving prescription capture rate requires more than isolated workflow adjustments. It demands cross-functional coordination and shared accountability.
A sustainable strategy shifts organizations from reactive recovery to proactive revenue protection.
Moving from reactive recovery to proactive revenue protection
Rather than identifying leakage after month-end reporting, proactive organizations embed predictive monitoring into daily workflows. This approach reduces preventable loss before it impacts financial statements.
Over time, this shift stabilizes revenue performance and reduces operational volatility.
Aligning pharmacy, finance, and operational teams around shared data
Enterprise improvement depends on alignment across departments. Pharmacy teams, finance leaders, and operational stakeholders must operate from a common data foundation.
Effective alignment includes:
- Shared dashboards that standardize capture rate metrics
- Clear definitions of high-value medication categories
- Agreed-upon escalation workflows for at-risk scripts
- Transparent reporting that links capture performance to financial outcomes
When teams share visibility and accountability, improvement efforts become coordinated rather than fragmented. This alignment strengthens both financial oversight and operational execution.
Strengthening Prescription Capture with Data-Driven Intelligence
As specialty therapies grow in cost and complexity, preventing prescription leakage becomes a strategic priority. Sustainable improvement requires technology that supports proactive insight and structured intervention.
Modern script capture strategies focus on:
- Real-time identification of at-risk prescriptions
- Intelligent prioritization of high-value therapies
- Enterprise-wide visibility across systems and sites
- Actionable insights embedded into daily workflows
Quva BrightStream Script Revenue Capture solution is purpose-built to help health systems protect prescription revenue across the medication lifecycle. By delivering centralized analytics, prioritized alerts, and measurable performance tracking, Quva BrightStream enables pharmacy leaders to move from reactive reconciliation to proactive revenue protection.
Turning Prescription Capture into a Strategic Advantage with Quva
Prescription capture rate is not simply an operational metric. It is a reflection of how well a health system coordinates data, workflows, and cross-functional teams to protect high-value medication revenue. Without real-time visibility and structured analytics, leakage remains hidden until financial performance declines. Traditional, retrospective approaches cannot keep pace with the complexity of specialty therapies and multi-site health systems.
Quva BrightStream Script Revenue Capture solution equips organizations with the intelligence needed to identify at-risk medication, prioritize high-value opportunities, and intervene earlier in the medication lifecycle. By aligning pharmacy, finance, and operational teams around shared data, health systems can improve capture rate, stabilize revenue, and strengthen long-term sustainability.
Sources:
- Elchehimi A, et al. Impact of pharmacist-driven referral to increase specialty pharmacy prescription capture. American Journal of Health-System Pharmacy. 2024;81(Suppl 2):S61–S67.https://academic.oup.com/ajhp/article-abstract/81/Supplement_2/S61/7633011
- Chmielewski GC, Cesarz S. A framework to increase prescription capture from health-system clinics. American Journal of Health-System Pharmacy. 2020;77(8):658–663.https://academic.oup.com/ajhp/article/77/8/658/5803147
- Michaud J, et al. Improving prescription capture rates through a standardized Meds to Beds program. Journal of Pharmacy Practice and Innovation. 2025.https://www.sciencedirect.com/science/article/pii/S2949969025000594
- Drug Channels Institute. Fresh Evidence: How Health Systems Steer Prescriptions to Their Own Pharmacies. https://www.drugchannels.net/2021/10/fresh-evidence-how-health-systems-steer.html

